
Hey mamas! After Micah was born I found myself reading his story over and over, but Katie’s sat untouched in a dusty corner. It’s was a “just the facts, ma’am” catalog of timestamps and pushing techniques . . . pretty much a total yawner. Now, I LOVED her birth, it was just that my story didn’t do it justice. So here is my second attempt: Elvis and Smurfs included for dramatic effect 🙂

In my bedside table there is a calendar with your conception date circled on it. That is a fact. Doing the potty dance in the Walgreens checkout line while holding a pregnancy test was just a formality . . . I knew you were there three days in when I ate an entire jar of olives and drank the juice!
And because I did the math – oh, about a thousand times – I can tell you it is also a fact that your due date was December 8th.
So when December rolled around I washed your little onesies and yellow ducky receiving blankets (we didn’t know if you were a boy or girl), made snacks for my birth attendants (which I, um, ate before they arrived), and waited.
tick. tick. tick.
tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick. tick.
Now Honey . . .
As much fun as it was to watch the gym staff clutch their chests as I heaved my planet-sized belly onto the stairmaster at 41 weeks, I was beginning to think we had a problem. A huge, 25th of December type problem. As you know, mama LOVES Christmas, but I couldn’t shake the feeling that I’d stuck you with a lemon of a birthday. Not ON Christmas, of course, but just close enough that your big day would be swallowed up in the hullabaloo. Now that I’ve gotten to know you a bit I see how silly this was. I mean, who could ignore this?!?!?

But I am getting ahead of myself. On the morning of Dec. 21, which was the final day of week number 42, you started revving things up around 6am. Of course, I promptly did what any reasonable laboring mother would do . . . I put rollers in my hair and grabbed my eyelash curler! A few days before I’d done a glam birth trial run, so I was pretty sure I had this in the bag.

Please feel free to skip ahead a couple paragraphs and laugh yourself silly at my naivete! So where were were we? Oh right, go time! I spent the morning wrapping Christmas presents and trying to stay relaxed. Then around midmorning my STRONG hypnobirthing “pressure waves” subsided into tiny ripples that barely lapped the shore. I was devastated, but now I’m glad I got a little rest before stage two.
Stage 2: Puke-A-Thon
So here is the thing about glamorous births: They do NOT involve heaving everything you’ve eaten since 1987 into a giant mixing bowl.
For 12. hours. straight. Current theories on how I was able to find enough stuff in my stomach to vomit after every other contraction include:
- I can metabolize air
- It was not really 12 hours, but one hour which I experienced Groundhog Day style (this conspiracy theory is patently false)
- I am Elvis
Whatever the true cause, my glam birthing clothes are covered in slime and I now have this ratty old t-shirt on.
By this point I’ve been awake for over 24 hours and haven’t been able to keep food or water down for half of that. I’m beyond weak and terrified that I don’t have the strength to finish. My midwives, Susan (aka The Urban Poser’s MIL) and Angela are becoming concerned for the very same reason.
Game Face? Check!
I needed some space from all the eyeballs gazing at me with deeply concerned expressions, so I took a shower. My family took this opportunity to hold full-on Sunday-go-to-meetin’ prayer extravaganza. They knew something had to happen or I was going to end up at the hospital with an emergency c-section.
Standing in the shower, I knew it too. But as steam swirled all around something changed. I was ready and willing to trust my body. My expectations of a picture-perfect birth with neatly coiffed hair and just the right shade of lip gloss were replaced by sweat and puke. But I was ready. Instead of running from the pain I started leaning into it, using this excruciatingly painful maneuver to cause myself to dilate. It worked.
Now, a funny thing about midwives is that they speak grunt. “Mhmmpf” means someone please hand me one of those oatmeal creme pies. But “Mmmmmmhmpf” is best translated as “fill the birthing tub now or I will have this baby standing up.” Since I’m clearly saying the latter by this point they fill the tub and help me in.
Ahhhhhhhhhhhhhh! After 35+ hours of labor this was exactly what I needed. Unfortunately I must have let out a “Ohmmpf,” which unbeknownst to me means “get me out of the tub so I can push on the toilet,” so out I came.
Oops.
Sitting backwards with my forehead on the tank did help, though, so I guess the midwives grunt translator is pretty accurate. Or maybe the Smurfs told them. Hey, who invited Smurfs to my birth!?!?!?
Susan didn’t see the Smurfs, but that’s probably because her perception had been dampened by the fact that she’d slept in the past 40 hours. Or I hallucinated them. Whatev.
So Here We Are . . .
Past the glam curler phase, the puke vortex and the Smurf interlude. I guess the only thing left is to push you out! Susan and Angela led me back to the birthing tub where your dad was waiting. I pushed, and pushed, and PUSHED, but all I got was a bulging bag of waters. Finally in desperation I asked my midwife to break it. The first tried and couldn’t, but the second was finally able to. (Susan later told me that my amniotic sac was incredibly strong because of the way I’d nourished myself through pregnancy. Yay me!)
With one gush I passed into the eye of the storm. Everything around me was suspended, and my only thoughts were of you. I felt no pain as you passed through, and as your Daddy gathered you up from the water I leaned back, exhausted. They laid you on my chest and I gazed at you in stupified amazement.
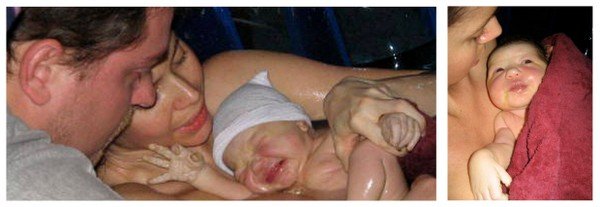
All through my pregnancy I had eaten well, exercised, etc. I had done everything I could to take care of you. But the moment I saw you I was totally undone. Your pink cheeks, rosebud mouth and tiny frame melted me into a puddle of awe. Finally your dad said “Well, what is it?” I had forgotten to check! We pulled back the towel and I yelled “It’s a GIRL!!!” just like in the movies.

We snuggled into a freshly-made bed and nursed while the midwives examined my placenta. Someone put a diaper on me and that was that. We were officially a family of three.
You were born three days before Christmas, and for years I felt guilty about it. But you know what? Your birthday is only time the sun rises and sets in the same place. Oh yes, little one, you are a Winter Solstice baby – wrapped in the paradox of a sun that appears to stand still right before the longest night of the year. From that day forward the days grow warmer and brighter until midsummer when all settles down for a quiet rest again.
The longest, darkest night followed by light and warmth? Yes, that sounds vaguely familiar! And that, sweet girl, is why I will never feel guilty about your birthday again. Indeed, it is the only day fitting for you.




