
Absentmindedly saying “I love you” when hanging up with a customer service rep because you’re also making dinner and signing for an unexpected package? Totally normal. Feeling the need to recharge after a move, a birth, a job change, or a family crisis? Also normal.
Feeling tired and stressed most of the time, with bouts of irritability and brain fog? Not normal, even if your lab results are. Last week, molecular geneticist and Functional Diagnostic Nutrition Practitioner Dr. Natcha Mathai and I shared some of the most common symptoms of hormone imbalance. Today, we’re going to cover why “normal” can be such a tricky thing to identify with lab tests, then look at some options for getting a clearer picture of what’s going on.
Before we jump in, please keep in mind that this article is for informational purposes only and is based on the opinions of the authors. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please see my full disclaimer here. Okay, let’s jump in!
So your hormone test results are normal, but you have symptoms of hormone imbalance? Let’s look at three common problems with hormone lab tests:
Problem #1: The “normal” lab test conundrum
You keep using that word. I do not think it means what you think it means.” – The Princess Bride
To understand the “normal” lab test conundrum, let’s take a look at one test that has received a lot of attention lately. The thyroid stimulating hormone test (commonly called the TSH test) was supposedly developed by taking samples from people who don’t have thyroid disease, then creating a normal range based on their numbers. If your numbers are lower or higher than the reference range, they’re considered abnormal.
Problem is, a lot of people who were thought to be “normal” in the sample group went on to be diagnosed as hypothyroid. (source) That’s not surprising since roughly 20 million people have some form of thyroid disease, but 60% don’t know it. (source)
It is problematic, however, because including individuals with thyroid dysfunction in the sample group means that what’s considered normal doesn’t necessarily reflect a state of health.
When imbalances occur it can take awhile to become glaringly obvious on a diagnostic test, but that doesn’t mean we should wait until then to pay attention to what our bodies are telling us.
Or, as Harvard educated gynecologist Dr. Sara Gottfried puts it:
You see, in mainstream medicine, we tend to have either/or thinking. Either your liver is working or you have liver disease. Either your thyroid is working or you have thyroid insufficiency. Either your adrenals are working or you have adrenal failure. There is rarely a ‘middle ground.’ The trust is that most of us exist in a wide range between those two extremes, which I call dysfunction or dysregulation. I believe it’s not only worthwhile but ultimately your responsibility (along with the help of a trusted clinician) to intervene before your organs become diseased. Intervention before failure, before insufficiency, is proven to contribute to lasting health and longevity.” – The Hormone Cure
The takeaway here is that instead of looking for “normal,” we need to be looking for optimal.

Problem #2: Hormones are present, but the cells are “locked”
According to Dr. Gottfried, “Due to hormone resistance, sometimes what you feel is not reflected in the blood, urine, or saliva level of a hormone. Your felt experience correlates with the hormone levels inside your cells, and especially inside the nucleus of your cells, which is where your hormones interact with your DNA (your genetic code).”
She goes on to say that our cells have hormone receptors that fit our hormones like a lock fits a key. If the lock is broken or jammed for some reason, your hormones don’t make it into cells where they are needed. In other words, we can have adequate production of a certain hormone and still have an issue because our cells can’t access them. Hormone resistance can occur with many hormones, including insulin, cortisol, progesterone and thyroid hormones. (Source: The Hormone Cure)
Problem #3: There isn’t one perfect test (unfortunately)
The journey of a hormone molecule looks something like this:
- It gets produced from the endocrine gland (e.g. ovary, adrenals, thyroid).
- It is released into the blood stream and bound by a type of protein called globulin.
- It travels to the target organs where it functions.
- It binds to the receptors on the surface of the cell.
- It tells the cells to change gene expression (cellular production) or how the cells behave.
- The liver or the gut bacteria convert it into other forms (metabolites), which may be more or less potent than the original hormone.
- The gut may also reabsorb these hormones back into the circulation.
We have hormones in the blood, in our cells, and in our gut. In the blood, our hormones can be bound to a protein or free, and only the free hormones will do the job.
When any of these processes go awry, symptoms of hormone imbalance can occur. If the right form of hormones or metabolites is not considered in the lab test, it’s possible to have “normal” numbers even when there’s a problem.
Unfortunately, there is not one test that can tell you everything, so you need a skilled practitioner that can look at potential issues with production (how much you make), transport, sensitivity (the jammed locks we talked about in #2), and detoxification (how well our bodies break down excess hormones), then look at your results and make sense of them.
Note from Heather: I’ll tell you more about why later in this article, but I’m actually working with my co-author, Dr. Mathai, to see what more I can do to optimize my hormone levels. The test I’m going to be using can be done at home and doesn’t require a blood draw.
My local holistic M.D. is ordering it for me so that it will most likely be covered by my insurance, but because of her expertise on balancing hormones, I’ve asked Dr. Mathai to help me work through and make sense of my results. If you’re interested in working with her as well you can find more information here. (She can also order labs, so if you don’t have a local doctor that you love working with, she can have the test sent to you. Also, if you mention this post and you’ll get $25 off your test.)

When and Why We Should Test for Hormone Imbalances
Ideally, it’s best to test hormones on a regular basis when you feel amazing, with zero symptoms, so that you have a baseline that reflects what “normal” looks like for you.
While most lab tests come with a reference range or a suggested optimal range, the sample used to determine that range may in some cases include individuals with a relevant type of dysfunction. Plus, everyone is different, so it makes sense that the optimal number for one person during a particular stage of life might be different from another.
If you are testing regularly, then you can tell something is starting shift if numbers veer from your optimal numbers. Sometimes you may be able to connect the shift with a lifestyle factor, stressful life event, dietary changes, or just the normal shift that occurs during different life stages. Other times, it just means that more investigation might be necessary.
Because hormone testing costs money, most people only get their hormones tested when a practitioner or doctor has reasonable grounds to believe that the tests will identify a problem. In this case, if you are experiencing symptoms of hormone imbalance and would like to get to the root of it, getting your hormones tested can often be helpful.
However, hormone imbalances are often a manifestation of stress in other systems in the body, which can be caused by diet, lifestyle factors, inflammation etc. When that’s the case, it’s vital to address those problems first as part of a holistic approach to healing.
Real-life note from Heather: If you’re thinking, “Whoa, I never thought to check my hormones while I felt great,” join the club! My hormones shifted after my third child was born. With my first two children I returned to my pre-pregnancy weight easily – not so with baby #3! I also struggled with HPA axis dysfunction, which is commonly known as adrenal fatigue.
Because my symptoms were relatively mild I didn’t think to test my hormones. Instead, I worked to heal my HPA axis dysfunction using these techniques. Later on, after my son weaned, I used the questionnaire from The Hormone Cure – which as I mentioned earlier was written by Harvard educated gynecologist Dr. Sara Gottfried – to identify lingering imbalances. (FYI, pregnant and breastfeeding mamas have different hormone patterns, and Dr. Gottfried’s book does not address them.)
After taking the quiz I implemented some of her suggestions along with a few others I discovered in my own personal research. My stress tolerance increased, I felt more ready to take on each day, and my body went back to the weight that’s normal for me. However, based on the questionnaire in Dr. Gottfried’s book there’s still room for improvement, so I’m working with my co-author, Dr. Natcha Mathai, to see how I can optimize them further.
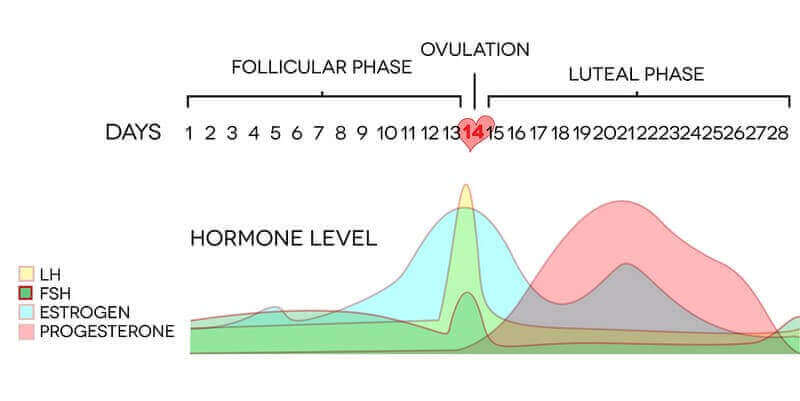
How do fluctuations in hormone cycles affect results?
With the exception of fertility cases, doctors are often reluctant to order hormone testing for women because it varies so much. Every month, our hormones – estrogen, progesterone, testosterone, FSH, and LH for example – fluctuate greatly, so getting a blood draw on any given day won’t give a complete picture.
In addition, more than 50% of premenopausal women use some form of hormonal birth control, so the results have to be interpreted by taking this into account. Because it is so confusing, it’s usually not very informative.
There are two solutions to measuring hormonal health, given the understanding that it fluctuates wildly.
1) Do a Cycle-Mapping Test
If you have symptoms that fluctuate with your cycle, it could be because some of your hormones don’t rise or fall correctly.
By collecting samples every day or every other day throughout the month, you can map out your hormone levels throughout the month and see whether hormone levels or monthly changes are an issue. That way, it is possible to design a natural support protocol for specific days of the month to nudge the hormones into the right place.
2) Take the Test Mid-Cycle
Just after ovulation (around day 18 – 22 of your cycle), your hormone numbers should be just about at their highest point, although progesterone may rise a bit more later on. Any abnormality at this point in your cycle is very informative.
While taking the test only once is less informative than mapping out the cycle, a single test mid-cycle of cortisol and sex hormones can help you determine
- How much your stress level is affecting your hormone levels
- How much reserve you have for stress
- Whether you have estrogen dominance
Options for Hormone Testing
Although there is no perfect test, it is possible to get a lot of useful information from labs. Here are some of the pros and cons to consider regarding each test:
Blood Tests for Hormone Imbalance
Blood testing is the original method of testing for hormones, and you can usually detect many more hormones this way than testing other samples.
The Pros
- It is possible to test for many different types of hormones. These include FSH, LH, Thyroid Hormones, Prolactin, and Insulin in addition to sex hormones and cortisol.
- You can look at free and bound hormones, plus hormone-binding globulin levels.
- Doctors and medical professionals are more familiar with blood tests than other tests.
- Some tests, like this thyroid test, can now be ordered directly from the lab and done at home
The Cons
- Certain tests require you to visit a blood draw station or a doctor’s office.
- Getting pricked by a needle is stressful to the body. This might throw off cortisol levels and make the test inaccurate.
- The need to visit a blood draw station/doctor’s office makes it harder to perform tests that require multiple collections, such as the 4-point cortisol test or month-long hormonal cycle test.
Saliva Hormone Testing
We have hormones in our saliva, which is why we kiss (so our partners can give us some of their testosterone). Measuring saliva hormones is measuring hormones in action.
Salivary testing is available for sex hormones, cortisol, cortisone, and melatonin.
The Pros
- Collection is easy, making it possible to collect samples multiple times. This allows us to look at cortisol at 4 or 5 different times throughout the day (also called adrenal stress index test).
- Able to measure free hormones inside and between cells
The Cons
- Only measures free hormones, and not much else. For example, free cortisol is only 1% of total cortisol.
- Not generally recognized in conventional medicine, although there are studies that show that the results are valuable (source, source).
- Doesn’t look at all different hormone metabolites
DUTCH: Dried Urine Test for Comprehensive Hormones
Dried Urine Spot Test (DUTCH) involves dipping a filter paper into the urine before drying it off and shipping it to the lab. The DUTCH is gaining its popularity among functional medicine practitioners simply because it gives a lot more information about hormone metabolism and function than other types of hormone tests.
Note from Heather: This is the one I’ll be doing.
The Pros
- Measure all different metabolites of sex hormones. This makes it possible to determine whether there is a problem with specific aspect of hormone metabolism, including if you have trouble with methylation.
- Low shipping cost because you are not shipping liquid, and samples are more stable than blood or saliva.
The Cons
We are measuring hormones excreted in urine, which means we are measuring extra hormones rather than working hormones. However, the DUTCH test usually correlates very well with the salivary test.
This article was medically reviewed by Dr. Anna Cabeca, a gynecologist and obstetrician and a menopause and sexual health expert. As always, this is not personal medical advice and we recommend that you talk with your doctor.
Do you have a question about testing or balancing hormones naturally?
Leave it in the comments below!
About the authors: This article was coauthored by Heather Dessinger Dr. Natcha Maithai (PhD). Dr. Maithai is a Registered Holistic Nutritionist and Functional Diagnostic Nutrition Practitioner with a PhD in molecular genetics. After becoming frustrated with hormonal problems that went undiagnosed despite her best efforts, Dr. Maithai applied tools she learned as a cancer researcher to dive into available scientific literature and find a holistic solution. You can find her health insights, biohacking tips, and information about working with her on her website, Natcha Maithai.




