Here’s a fun little question for you – which one of these statements is true?
A) A Banyan Tree near Kolkata, India is larger than the average Walmart
B) There are more nerve connections in your brain than there are stars in our galaxy
C) Heartburn is usually due to too little stomach acid, not too much
Okay, that was a trick question. They’re all true. (1) Now, maybe you’re thinking, “That can’t be right. I’ve taken an antacid when I had heartburn and it helped, so clearly the issue was too much acid.”
That’s certainly what I thought when I was one of the 60 million Americans struggling with heartburn. However, according to Jonathan Wright, M.D., author of Why Stomach Acid Is Good For You, the “Chances are very high – over 90 percent – that the real culprit is actually underproduction of stomach acid.”
Unfortunately, the most popular form of over-the-counter medications – proton pump inhibitors – “are not the benign drugs the public thinks they are,” says Dr. Shoshana J. Herzig of Harvard Medical School. (2)
We’ll dive into why later in this article, plus what Dr. Wright says is the true cause of most heartburn, but first I want to mention that none of these statements have been evaluated by the FDA, this article is not medical advice, and it is not meant to diagnose or treat any condition. I’m just a former heartburn sufferer passing along information I’ve found helpful from respected physicians, clinical studies conducted by places like Johns Hopkins University, and articles from Scientific American and the Mayo Clinic.
Please talk with your healthcare provider about what approach to heartburn is best for you. Now that we’ve got that out of the way, let’s dive in.
So if antacids aren’t reducing excess acid, what are they actually doing?
According to Dr. Wright, who has worked with thousands of heartburn patients at the Tahoma Clinic:
“stomachs are built for the very purpose of containing and working with very strong acid, acid that is one-hundred-thousand times stronger than the acidity of our blood.” (3)
Our stomach acid plays an essential role in helping us break down food so that nutrients can be absorbed, and also kills a variety of bacteria, parasites, and other pathogens on contact. When levels are normal, individuals are very unlikely to experience heartburn symptoms such as a bitter, acid taste in the mouth or a burning sensation in the throat or behind the breastbone.
However, if acid levels are low, the chances increase. Here’s why:
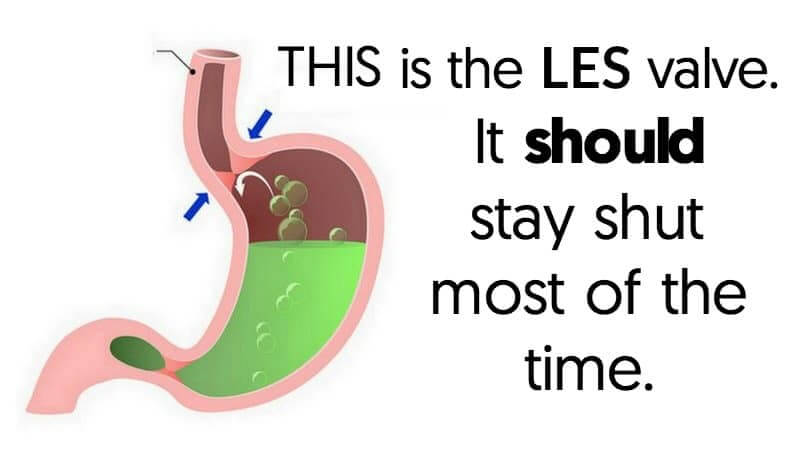
Just above the stomach there is a valve called the lower esophageal sphincter (LES) – it protects the esophagus from harsh stomach acid. When the LES is functioning normally, it only opens when you eat, drink, belch, or (yep) vomit.
If the LES is working properly, it doesn’t matter how much acid we have on our stomachs. It’s not going to make it up to the esophagus. On the other hand, if the LES is asleep at the switch, even a small amount of acid could reflux into the esophagus under the right conditions. Scientists have found that when we have heartburn or GERD, the LES opens briefly when it’s not supposed to. If we’ve got acid – or anything else – in our stomachs, sometimes even a little bit, and it happens to be in the vicinity of the LES when it pops open inappropriately, we get reflux.” (3)
So what causes the LES to malfunction?
After testing the gastric pH of thousands of heartburn sufferers at his Tahoma Clinic, Dr. Wright has concluded that in 90%+ of cases it’s low stomach acid that is causing LES malfunction.
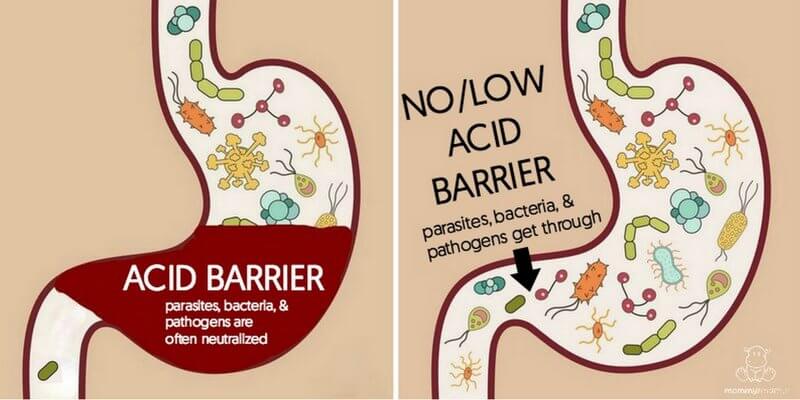
Remember, in addition to breaking down food so that nutrients can be absorbed, stomach acid also provides an “acid barrier” that kills bacteria, parasites, and other pathogens in our food.
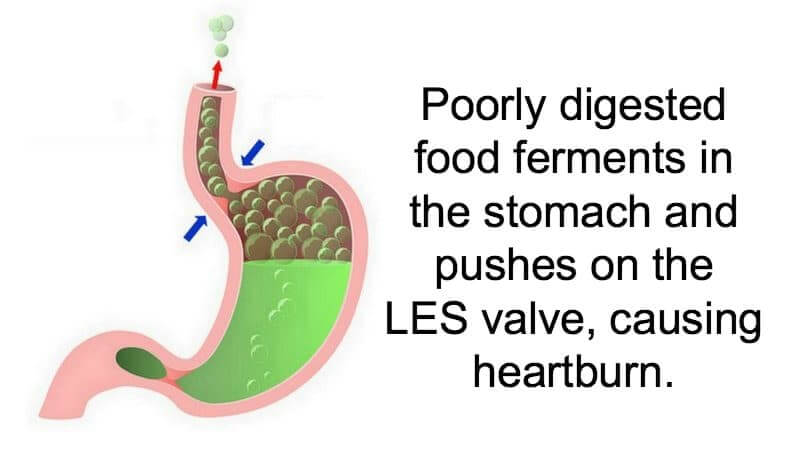
If the acid is too weak, poorly digested food – especially carbohydrates – can become a source of nourishment for these bacteria/pathogens. As they feed, they produce fermentation byproducts (gases) that create pressure in the stomach and push on the LES valve. When the pressure builds, some acid may be pushed through the LES into the esophagus, causing heartburn.
Stomach acid levels tend to drop as we age, so if heartburn were caused by too much of it you’d think this would mostly be an issue for kids and teens. Of course, it’s the opposite.
That’s not to say teens can’t have low stomach acid – I actually got my first prescription for heartburn when I was nineteen. But on the whole, we tend to have more problems with heartburn as we get older despite dropping levels of stomach acid.
Dr. Wright’s “argument is with the mistaken concept that it takes ‘too much’ stomach acid to do the damage. Even a small amount of acid in the wrong place (such as the esophagus) can cause symptoms and ultimately tissue damage. (After all, we know that stomach acid is strong stuff, if it can help reduce a tough beefsteak into the equivalent of beef soup in an hour or so.)” (3)
In some cases a hiatal hernia – which is when the upper part of the stomach bulges through the large muscle separating the abdomen and chest – can also cause LES dysfunction. For some people chiropractic care may be able to ease the stomach back into its proper place, and in other cases surgery may be required.
Hiatal hernias can be diagnosed with an endoscopy, which allows the doctor to look at the area directly or an X-ray that requires the patient to take barium (which is a heavy metal). Personally, I’d opt for the endoscopy.
Calcium channel blockers can also lower esophageal sphincter tone, making the LES more susceptible to dysfunction. (4)
Common Causes of Low Stomach Acid
- Age (levels tend to drop over time)
- Stress, particularly the chronic type, can inhibit the body’s secretion of hydrochloric acid (stomach acid). (5)(6)
- Certain gut infections, such as H. pylori and candida, reduce the body’s production of hydrochloric acid (7) It can be argued, however, that these infections only take hold if gastric acid secretion is already compromised. From that perspective, the presence of these microbes simply further inhibits the production of hydrochloric acid.
- A mutation in one of the genes that influences gastric acid production (8)
- Use of antacid medications
Heartburn Medication Concerns
Most of us tend to think of heartburn medications as pills that just “take the edge off” and leave us with normal acid levels. Unfortunately, not only can they reduce levels that may already be too low, sometimes they almost completely eliminate it.
The drug most commonly prescribed for heartburn today, Prilosec, virtually eliminates acid in the stomach around the clock, a fact that is proudly promoted in the drug’s widespread consumer-oriented advertising. Prevacid, Aciphex, Protonix and Nexium do about the same thing.” (3)
Although eliminating stomach acid will relieve symptoms of indigestion, it also prevents the stomach from doing its job – digesting food and killing pathogens as they enter our system. When taken long-term – which is defined as more than one year by the FDA – heartburn medications may cause side effects such as decreased resistance to infection, nutritional deficiencies and an increased risk of certain diseases.
Impaired Resistance To Infection
As we covered earlier, the stomach is supposed to be an “acid barrier” that protects against intestinal tract infection. Unfortunately, according to John Clarke, a gastroenterologist at Johns Hopkins Hospital in Baltimore, lowering stomach acid using proton-pump inhibitors like Nexium, Prilosec and Prevacid “leaves people vulnerable to nutritional deficiencies and infections, including food poisoning like salmonella, a serious, sometimes life-threatening digestive system infection called Clostridium difficile, and perhaps pneumonia.” (9)
Other studies have found individuals who take acid suppressing drugs have an increased risk of getting pneumonia. (10)
Dr. Wright tells this story:
Here’s an extreme, but very revealing, incident: Decades ago, public health officials in India investigated why some people in a village in the midst of a cholera epidemic didn’t contract the disease, while others did. They found that more of those who stayed healthy had normal levels of stomach acid, while those that developed the disease usually did not. Apparently, the strong stomach acid killed the bacteria before it could ‘colonize’ (and damage) the entire gastrointestinal tract.” (3)
Decreased Nutrient Absorption
Stomach acid helps to cleave vitamins and minerals away from dietary fats, proteins, and carbohydrates. Without it, our bodies don’t break nutrients down in absorbable pieces, which can lead to deficiencies – even when someone is eating a very healthy diet. Studies have found connections between acid blocking medications and low levels of:
- Vitamin B-12 (11)
- Vitamin C (12)
- Iron (12)
- Magnesium (2)
Conditions Associated With Low Stomach Acid
Inadequate levels of stomach acid have been associated with a number of health conditions, including:
- Allergies (13)
- Anemia (13)
- Asthma (13)
- Autoimmune diseases such as Rheumatoid arthritis and Graves disease (13)
- Chronic kidney disease (14)
- Dementia (15) (16)
- Heart attack (17)
- Heartburn/acid reflux
- Skin issues such as acne, eczema or psoriasis (13)
- Small intestine bacterial overgrowth (SIBO) (18)
- Stomach cancer (19)
Research suggests low stomach acid may also increase the risk of:
- Diabetes (20)
- Chronic liver disease (21)
- Osteoporosis (22)
Lifestyle Changes That May Help
According to Dr. Jonathan Wright, “In cases of mild to moderate heartburn, ‘acid indigestion,’ bloating, and gas, actual testing for stomach acid production at Tahoma Clinic shows that hypochlorhydria (too little acid production) occurs in over 90 percent of the thousands tested since 1976.
In these cases, a ‘natural strategy’ is almost always successful.” (3)
You’ll find the details of his approach in this article.
This article was medically reviewed by Madiha Saeed, MD, a board certified family physician. As always, this is not personal medical advice and we recommend that you talk with your doctor.
Want more research-backed natural remedies?
No problem, I’ve created a free ebook for you – Kitchen Apothecary: 25+ Natural Remedies Using Ingredients From Your Pantry – as a gift for signing up for my newsletter. You’ll also get updates when I post about safe essential oils for pregnant/breastfeeding mamas, exclusive gifts and coupons (I was able to give away a jar of free coconut oil to anyone who wanted it recently!), plus other goodies.
Sign up using the form below.
Sources
1. Insider (2014) 17 Crazy Facts That Sound Fake But Are Actually True
2. New York Times (2015) Taking Heartburn Drugs Long-Term
3. Wright, Jonathan (2001) Why Stomach Acid Is Good For You
4. Seretis, Charalampos et. al. (2012) Calcium Channel Blockers and Esophageal Sclerosis: Should We Expect Exacerbation of Interstitial Lung Disease?
5. Esplugues, J. V. et. al. (1996) Inhibition of gastric acid secretion by stress: A protective reflex mediated by cerebral nitric oxide
6. Kelly G. Lambert and Craig H. Kinsley (2010) Clinical Neuroscience: Psychopathology and the Brain Second (2nd) Edition
7. Brzozowski, Tomasz et. al. (2005) Influence of gastric colonization with Candida albicans on ulcer healing in rats: effect of ranitidine, aspirin and probiotic therapy
8. Science Daily (2008) Gene That Helps Control Production Of Stomach Acid Discovered
9. NPR (2016) Popular Heartburn Pills Can Be Hard To Stop, And May Be Risky
10. Laheij, Robert J. F. et. al. (2004) Risk of Community-Acquired Pneumonia and Use of Gastric Acid–Suppressive Drugs
11. Mayo Clinic. Heartburn medicines and B-12 deficiency
12. Heidelbaugh, Joel J. (2013) Proton pump inhibitors and risk of vitamin and mineral deficiency: evidence and clinical implications
13. Medical News Today. What is hypochlorhydria?
14. Washington Post (2016) Popular heartburn medication linked to chronic kidney disease
15. New York Times (2016) Heartburn Drugs Linked To Dementia Risk
16. Science Daily (2020) Newly discovered mechanism can explain increased risk of dementia
17. Stanford Medicine (2015) Some heartburn drugs may boost risk of heart attack, study finds
18. Dukowicz, Andrew C. et. al. (2007) Small Intestinal Bacterial Overgrowth
19. New York Times (2017) Heartburn Drugs Linked To Stomach Cancer Risk
20. Diabetes Research & Wellness Foundation. Stomach acid could protect people from type 2 diabetes
21. National Institutes of Health (2017) Blocking stomach acid may promote chronic liver disease
22. Pentti Sipponen and Matti Härkönen (2010) Hypochlorhydric stomach: a risk condition for calcium malabsorption and osteoporosis?





Thanks for the article Heather! I’m looking forward to the follow up. I’ve had Acid Reflux/GERD for many years (15+) and have taken PPIs for years (15+). I know these are very bad, but w/o I’m constantly nauseous and even gag during workouts or levels of high energy. I’m unable to sleep and all I want to do is eat in order to try to ease the ‘burn’. I’ve been reading Chris Kresser’s blog post for a while trying to work through this. I eat very healthy (Paleo, no grains) and incorporate probiotics, kraut and kombucha into my diet, but I’ve still had no luck. I go next month to get a stomach scoop to see if there’s any issue w/ my LES Valve. That being said, I remember my mother having extreme heart burn, also, do you think this can be hereditary? I really really enjoy your blog and post, thanks again!!!!!
Hi
I have had it for years. I started drinking Aloe Vera… It is gone, gone. I mix it in Cranberry juice or anything really and take my water bottle with me. If for some reason I feel it is coming on I will take a coupe of ounces straight. In seconds no burning. Aloe Vera is good for u on many levels.. Try it.. U will be amazed.
Cheers
Carol Ann
I will give it a try!!!! Thanks!
My daughter Mary Strain works for a Dr Mark Noire in Towson Md who has pioneered a technique where he repairs (lazers) faulty valve. Within a year most people are off their meds.
That’s exciting! My husband just had the Lap surgery and although he is better, burps alot and has to eat very slow. I guess that’s a good thing, though to eat slower…Keep us posted on any new details of that.
Hi,please try “Siberian Pine Nut Oil”…it did help me,that is the only and aloe vera juice I was using
Eat slowly.
Chew well, very-very well.
Find peace in your life. A stressed person is a stressed GI tract. That means the GI tract is tight and anxious, not a good space to be digesting food in.
Slowly wean off PPIs and slowly rebuild your stomach acid back to normal with apple cider vinegar drinks.
Ease the burn with sips of aloe juice or apple slices. find what works for you.
Be patient with the process.
Hi my son had bad chicken at a restaurant 2years ago and he is still suffering with stomach issues they told him he now has slow digestion. But he has the same symptoms as you with working out he will throw up he can’t eat anything spicy. He can only tolerate a few bites out of a banana and yoghurt in the morning. In my family my father,sister and I all have stomach issues so I wonder if it’s hereditary? I will try the aloe Vera and see if it helps we do eat healthy so I’ll put it in our smoothies. Thanks for the tips!
By using Jacky sionu new technique no more heartburn, it work for everyone, and he is on the facebook.
Fascinating info! Now, how can I educate the geriatric doctors and all my long-term care patients? 😐
I’ve used nexium for several years, before that I took prilosex and before that zantec. So tired of this. I hand an inflamed gallbladder which had to be removed.
Very interested in hearing your solutions. My mom would take digestive enzymes to help with hers.
I have been reading lots of homeopathic information, and my favorite homeopath, Joette Calabrese (JoetteCalabrese.com) says that much of the heartburn can also be traced back to use of antibiotics. She has a protocol that (long term) will help remedy the heartburn.
However, many people coming off PPIs (my husband is one) cannot come off them cold-turkey; it causes a major upsurge in acid production and make you feel even worse than before you started them.
Good luck to everyone who wants to come off them – I am looking forward to the next article.
Looking forward to your follow-up on how to reduce heartburn. I am on 40 mg of nexium twice daily. I am at a point now where I experience esophagus spasms which feel like a heart attack and extremely painful. The last attack lasted more than 24 hours.
Correction: 40mg of Nexium twice daily
Thank you so much mummy. Great information.
Interested in alternatives to
PPI medication.
Thanks!
Love your posts ! Am wondering…have you heard of Shonishin non-inserted Pediatric Acupuncture? [ see Acufinder article from some years ago: https://www.acufinder.com/Acupuncture+Information/Detail/Shonishin+Acupuncture+for+Children ]
It may be a topic of interest for you.
best wishes,
Brenda
Very good article! My father has been taking strong meds for several years and now I think his stomach just stops functioning. I’m so much looking forward to your suggestions on natural remedies.
makes a lot of sense – if ever (very seldom as in less than once/year) I get heartburn and drink some ACV it goes away on the spot. Waiting for the next post! 🙂
Thanks for the article! My son (now 17) had a terrible case of H. pylori when he was about 5 or 6 yrs old. He had reached the point that he could keep very little food down and was always sick. A specialist found his extremely high H. pylori numbers and put the entire family on an antibiotic and heartburn medicine regime (supposedly we could contract it from my son’s saliva). This was over 10 years ago and I distinctly remember the bill, with insurance, being over $100 for each person! Everything was fine for about a week after the regime ended and then we were right back to the beginning. Fortunately, we somehow stumbled upon a chiropractor that put my son on a HCL supplement with this same explanation of how he needed more stomach acid to fight off the H. pylori invasion. He was right too! I praise the LORD that He directed us to someone that knew how to help the body heal itself instead of using unnecessary drugs.
My husband is on 40 mg of Nexium and has been for years. Every time he has tried to go off his heartburn comes back with a vengeance. We both hate these meds but at 80 would be thankful for a healthy alternative. Anxiously waiting for you follow-up article. Carole
I read your article on heartburn. My stomach problems sound quite a bit like yours. I did not see a date on your article, however, I did notice the first comment is dated August 14, 2016. Therefore, I suppose you have not published your follow up article yet. I am very anxious to read your follow up on heartburn. I hope we won’t have to wait too long for it. : ) Thank you for caring enough to let other people know about this.
I want to get off Nexium
Nexium has caused my parathyroid glands to leach calcium so now I have to take calcium citrate and magnesium supplements. Tired ofir
Hi Judy, when my parathyroid was leaching calcium, my doctor did a blood and urine test followed by an ultra sound of my four parathyroids as it can be a sign of a benign adenoma (Tumour) growing. In my case it was three adenomas and I had to have them surgically removed, all the symptoms went away after the surgery, I had 13 of the 15 symptoms. Life is much better now, there is a lot of information if you google it, it often goes undiagnosed for many years and it is most common for females over fifty.
Hi!
I can’t wait to read the followup to this. I have found that the only thing that helps mine is to be on an only meat, veggies and healthy fats diet. It’s driving me crazy. I miss fruit. My doctor is now testing me to see if I have a small intestine bacterial infection but from what I’ve read you take antibiotics and it still comes back. I’m curious how that kind of infection relates to low stomach acid?
Thanks for sharing this. I have shared now with several clients (and on FB) as this is easy to understand and right to the point.
I admit that I skimmed the article above…just want to encourage investigation of a link between antibiotic use and heartburn. I developed reflux and a yeast infection (in the throat, mouth, and vagina) after antibiotic use. A combination of oral antifungals, temporary use of omeprazole, digestive enzymes, colostrum, probiotics, and dietary changes finally rid my body of the infections. It took a year and a half, visits to several doctors (some provided misdiagnosis), and reading a book from the library about natural alternatives to omeprazole to finally cure me. So…if you get acid reflux after antibiotic use, clean up your gut.
Very interesting!
Had reflux for about 30 years. Until recently I have been on Omeprazole for most of that time. I just started taking 6mg of meletonin about an hour before I go to bed and that seems to taken my reflux away.
Very timely and interesting information! I look forward to the follow up. Thank you.
I’m interested in learning more!
I’m interested in the newsletter for improving stomach acid!
Interesting!
I have bad heart burn
Do you have any comment on Infant GERD? Does the same theory hold true? My eleven week old (who was born 4 weeks early at 35weeks 5days) has horrible reflux that has plagued us since she was two weeks old. We’ve tried Gaviscon, Zantac, and are now on to Nexium (all for infants, of course). We are starting Infant probiotics next week to see if that helps. Would love to get that ol’ esophageal sphincter to work properly as well!
I would like to get the info on reducing acid
Yes please send me info on heart burn & reflux.
interesting
Id like to get info too, please
Hi I am taking anti acid tablets frequently… your information would be of great help… thanks
I am starting to experience complications from years of taking nexium. I recently tried to stop taking it, but couldn’t. I’m interested in the information you offered
Sounds to good to be true.
Many posters talk about their long term use of antacids, but they are only for short term use. Some refer to their family genes, but while genes may give your family similar weaknesses, they rarely cause bodily issues unless taxed. Poor lifestyle may cause the same issue with blood relatives and a totally different issue with a non-blood relative of the same household. An interesting aspect about being overweight is that although it’s basically what (not how much) you eat and the condition of your gut microbiome, it is also influenced by what your grandmother ate while pregnant with your mother. Of course, your mother’s diet while pregnant and nursing plus many other items will also have an influence. Nevertheless, it is what you do that matters most.
There are many incompetent doctors prescribing obsolete drugs that promote:
Immune dysfunction
Digestion issues
Weight gain
Yeast infections and
Organ cancers
These antibiotics are still being prescribed to a naive public as if they were harmless.
Would love to get more info about this.
TY for emailing the article.
Interested in newsletter.
I would like the info please.
Just a note to say barium is not radioactive. It is dense so that x-rays don’t easily penetrate it, that’s why it shows up like bones do on an x-ray.
I would love to know more about stomach acid and how to raise it. I have chronic lyme… and multiple other health issues.
My stomach acid is extremely low. I have a very hard time digesting food. Lemons and salsa give me attacks that put me in the hospital. I had a colonoscopy and after 18 hours of not eating, my food was still undigested.
I want to learn about getting rid of acid reflux naturally
Looking forward to reading your newsletter!
Very interesting read.
I’d like to learn how to increase acid levels naturally.
Great post. Thank you.
Great info! Thanks!
I sometimes have stomach acid come up in my mouth when I’m sleeping and then you can’t breathe, scares the crap out of me, you have to keep swallowing and gasp for air till it passes. Is raw apple cider vinegar good for this? I have a hard time trying to swallow it even in water, it’s so strong. Can I take the pills instead? Please help me.
Will try it as soon as the healthfood store opens. For the infusion do you use the powder or the chopped herb?
D. Bogusch
Looking forward to learning more about increasing stomach acid
I really thank you for that information.
I have had ERGE for 17 years old, I am really tired and sick. My life has been a missery because there have been no useful medications for me. I have taken all kind of medicines (esomeprazol, lansoprazol, dexlansoprazol, omeprazol, levosulpiride, cinitapride, etc… and no improve has come to my life. The LES does not work and my throat is totally hurt, It is supposed that I do not have HP anymore, but I continue with ERGE. Almost all food causes acid reflux to me, even the valve between stomach and long intestine sometimes appears not to be working (in one of the 7 gastric endoscopy the doctor told me that I had alkaline reflux) I will appreciate if you send me information how to get better.
Would love some further information on how to treat heartburn.
Many Thanks
Melissa
Hi Melissa, you may find this post helpful
Heather, I love reading your posts on FB.
I’m wondering if this is how we request the info on getting off PPI’s?
Thanks!
Hello, I’m interested in how to treat heartburn. I really enjoy all the information you put out, thank you.
Please send me the info on how to treat heartburn naturally. Great info in your article above. Thank you.
You’ll find the article here: https://mommypotamus.com/how-to-get-rid-of-heartburn-naturally/
I want recipt eat